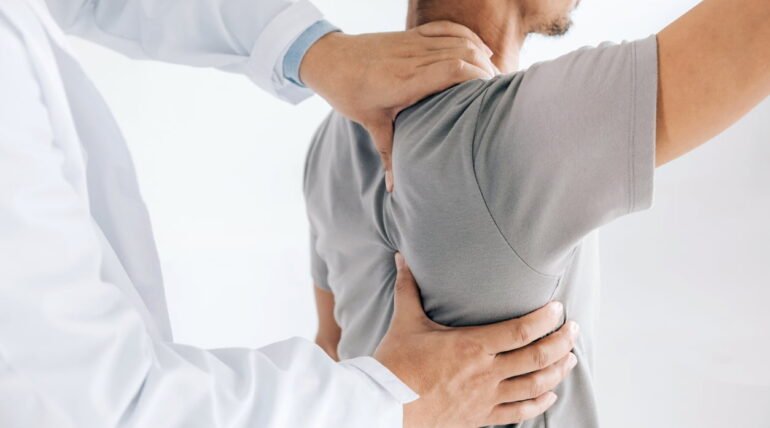
Joint mobilization is a manual therapy technique commonly used by physiotherapists to restore movement, reduce stiffness, and alleviate pain in restricted joints. By applying controlled, graded oscillatory or sustained movements to the joint, mobilization helps improve arthrokinematics, stimulate mechanoreceptors, and promote tissue healing. This article explores the principles, techniques, mechanisms, and therapeutic benefits of joint mobilization within modern rehabilitation practice.
Introduction
Joint restriction and stiffness are common consequences of injury, immobilization, or degenerative changes. These limitations can reduce range of motion, alter movement patterns, and increase pain during daily activities. While various interventions can target these issues, joint mobilization remains one of the most effective manual therapy approaches for restoring normal joint mechanics. It forms an essential part of both passive and active rehabilitation programs, often used alongside stretching, strengthening, and proprioceptive exercises.
Principles and Techniques
Joint mobilization involves rhythmic or sustained passive movements applied by the therapist within the patient’s pain-free range. The technique is typically classified according to Maitland’s grades (I–V):
- Grade I–II: Small or large amplitude oscillations within the available range, primarily for pain modulation.
- Grade III–IV: Larger amplitude movements into tissue resistance, aimed at improving mobility.
- Grade V (Manipulation): A small, high-velocity thrust beyond the end range to release joint restriction (performed only by qualified professionals).
The technique chosen depends on the treatment goal — whether to reduce pain, increase motion, or both.
Physiological Mechanisms
The therapeutic effects of joint mobilization arise through several mechanisms:
- Mechanical: Restores normal joint play, improves capsule elasticity, and reduces adhesions.
- Neurophysiological: Stimulates joint mechanoreceptors, inhibits nociceptive (pain) pathways, and reduces muscle guarding.
- Circulatory and Nutritional: Enhances synovial fluid exchange, promoting cartilage health and tissue nutrition.
- Psychological: Reduces fear of movement and increases patient confidence through gentle motion.
Clinical Benefits
- Pain Reduction: Mobilization decreases joint irritation and modulates central pain perception.
- Improved Mobility: Helps recover normal range of motion in hypomobile joints following injury, surgery, or immobilization.
- Enhanced Function: Better joint motion leads to improved performance in daily activities.
- Complementary Role: Works synergistically with active exercise therapy for long-term functional gains.
Applications
Joint mobilization is widely applied in treating conditions such as:
- Frozen shoulder (adhesive capsulitis)
- Neck and low back pain
- Post-immobilization stiffness
- Osteoarthritis and joint degeneration
- Sports-related joint restrictions
It is also valuable during post-operative rehabilitation, where restoring joint glide and accessory motion is essential for full recovery.
Conclusion
Joint mobilization remains a cornerstone of manual therapy, offering a safe and effective means of restoring movement and reducing pain. When combined with active rehabilitation and patient education, it enhances overall functional outcomes and accelerates recovery. Continued research supports its use as part of a multimodal approach to musculoskeletal rehabilitation, emphasizing both short-term pain relief and long-term functional improvement.

Moving the goalposts sorry i was triple muted, so what do you feel you would bring to the table if you were hired for this position. A better understanding
Neque porro est qui dolorem ipsum quia quaed inventor veritatis et quasi architecto beatae vitae dicta sunt explicabo. Aelltes port lacus quis enim var